Addressing the unmet need in NSCLC progression with advances in second-line therapeutics
Lung cancer is the leading cause of cancer mortality globally, with non-small cell lung cancer (NSCLC) accounting for 85% of cases. Despite advancements in first-line treatments such as immunotherap
[...] Read more.
Lung cancer is the leading cause of cancer mortality globally, with non-small cell lung cancer (NSCLC) accounting for 85% of cases. Despite advancements in first-line treatments such as immunotherapy and targeted therapies, resistance to these treatments is common, creating a significant unmet need for effective second-line therapies. This review evaluates current and emerging second-line therapeutic options for advanced or metastatic NSCLC, focusing on their efficacy and potential to improve patient outcomes. Anti-angiogenic drugs like ramucirumab combined with chemotherapy, particularly docetaxel, have shown moderate success. Antibody-drug conjugates (ADCs) targeting specific tumor antigens offer a promising avenue for targeted therapy, while chimeric antigen receptor (CAR)-T cell therapy and T-cell receptor therapy leverage the patient’s immune system to combat cancer more effectively. mRNA vaccines, although in early stages, show potential for inducing robust immune responses against cancer-specific antigens. Building on this foundation, recent advancements in molecular testing and the exploration of the tumor microenvironment are opening new therapeutic avenues, further enhancing the potential for personalized second-line treatments in NSCLC. While ADCs and bispecific antibodies are gaining traction, more precise biomarkers are needed to optimize treatment response. Regular monitoring through techniques like liquid biopsies allows real-time tracking of mutations such as EGFR T790M, enabling timely therapeutic adjustments. Additionally, the role of neutrophils and macrophages in the tumor microenvironment is increasingly being recognized as a potential therapeutic avenue, with Smad3 emerging as a key target. Further research into drug sequencing, toxicity management, and biomarker development remains crucial to improving NSCLC treatment outcomes.
Kinsley Wang ... Robert Hsu
View:266
Download:22
Times Cited: 0
Lung cancer is the leading cause of cancer mortality globally, with non-small cell lung cancer (NSCLC) accounting for 85% of cases. Despite advancements in first-line treatments such as immunotherapy and targeted therapies, resistance to these treatments is common, creating a significant unmet need for effective second-line therapies. This review evaluates current and emerging second-line therapeutic options for advanced or metastatic NSCLC, focusing on their efficacy and potential to improve patient outcomes. Anti-angiogenic drugs like ramucirumab combined with chemotherapy, particularly docetaxel, have shown moderate success. Antibody-drug conjugates (ADCs) targeting specific tumor antigens offer a promising avenue for targeted therapy, while chimeric antigen receptor (CAR)-T cell therapy and T-cell receptor therapy leverage the patient’s immune system to combat cancer more effectively. mRNA vaccines, although in early stages, show potential for inducing robust immune responses against cancer-specific antigens. Building on this foundation, recent advancements in molecular testing and the exploration of the tumor microenvironment are opening new therapeutic avenues, further enhancing the potential for personalized second-line treatments in NSCLC. While ADCs and bispecific antibodies are gaining traction, more precise biomarkers are needed to optimize treatment response. Regular monitoring through techniques like liquid biopsies allows real-time tracking of mutations such as EGFR T790M, enabling timely therapeutic adjustments. Additionally, the role of neutrophils and macrophages in the tumor microenvironment is increasingly being recognized as a potential therapeutic avenue, with Smad3 emerging as a key target. Further research into drug sequencing, toxicity management, and biomarker development remains crucial to improving NSCLC treatment outcomes.
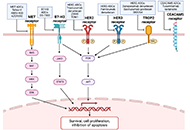 Addressing the unmet need in NSCLC progression with advances in second-line therapeuticsOpen AccessReviewLung cancer is the leading cause of cancer mortality globally, with non-small cell lung cancer (NSCLC) accounting for 85% of cases. Despite advancements in first-line treatments such as immunotherap [...] Read more.Kinsley Wang ... Robert HsuPublished: November 1, 2024 Explor Target Antitumor Ther. 2024;5:1297–1320
Addressing the unmet need in NSCLC progression with advances in second-line therapeuticsOpen AccessReviewLung cancer is the leading cause of cancer mortality globally, with non-small cell lung cancer (NSCLC) accounting for 85% of cases. Despite advancements in first-line treatments such as immunotherap [...] Read more.Kinsley Wang ... Robert HsuPublished: November 1, 2024 Explor Target Antitumor Ther. 2024;5:1297–1320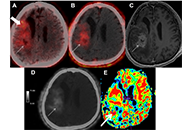 Preliminary evaluation of FAPI-04-PET/CT for differentiating recurrence and post-treatment changes in high-grade gliomasOpen AccessShort CommunicationFibroblast-activated protein (FAP) expression in glial cells is attributed to FAP-positive foci on tumor vessels and neoplastic cells. Preclinical and pilot studies have shown FAP expression in high [...] Read more.Indraja D. Dev ... Archi AgrawalPublished: October 31, 2024 Explor Target Antitumor Ther. 2024;5:1289–1296
Preliminary evaluation of FAPI-04-PET/CT for differentiating recurrence and post-treatment changes in high-grade gliomasOpen AccessShort CommunicationFibroblast-activated protein (FAP) expression in glial cells is attributed to FAP-positive foci on tumor vessels and neoplastic cells. Preclinical and pilot studies have shown FAP expression in high [...] Read more.Indraja D. Dev ... Archi AgrawalPublished: October 31, 2024 Explor Target Antitumor Ther. 2024;5:1289–1296 Predictive and prognostic biomarkers in cancer: towards the precision medicine eraOpen AccessEditorialStefano Marletta ... Luca FalzonePublished: November 20, 2024 Explor Target Antitumor Ther. 2024;5:1321–1325
Predictive and prognostic biomarkers in cancer: towards the precision medicine eraOpen AccessEditorialStefano Marletta ... Luca FalzonePublished: November 20, 2024 Explor Target Antitumor Ther. 2024;5:1321–1325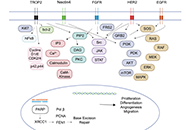 Targeted therapies and molecular targets in the therapeutic landscape of advanced urothelial carcinoma: state of the art and future perspectivesOpen AccessReviewAdvanced urothelial carcinoma (aUC) has a dismal prognosis, with a 5-year survival rate of approximately 10%. Platinum-based chemotherapy has been the backbone of the first-line treatment of aUC for [...] Read more.Irene Testi ... Ursula VoglPublished: November 21, 2024 Explor Target Antitumor Ther. 2024;5:1326–1364
Targeted therapies and molecular targets in the therapeutic landscape of advanced urothelial carcinoma: state of the art and future perspectivesOpen AccessReviewAdvanced urothelial carcinoma (aUC) has a dismal prognosis, with a 5-year survival rate of approximately 10%. Platinum-based chemotherapy has been the backbone of the first-line treatment of aUC for [...] Read more.Irene Testi ... Ursula VoglPublished: November 21, 2024 Explor Target Antitumor Ther. 2024;5:1326–1364